How Engineering Helped Reinvent the Artificial Knee
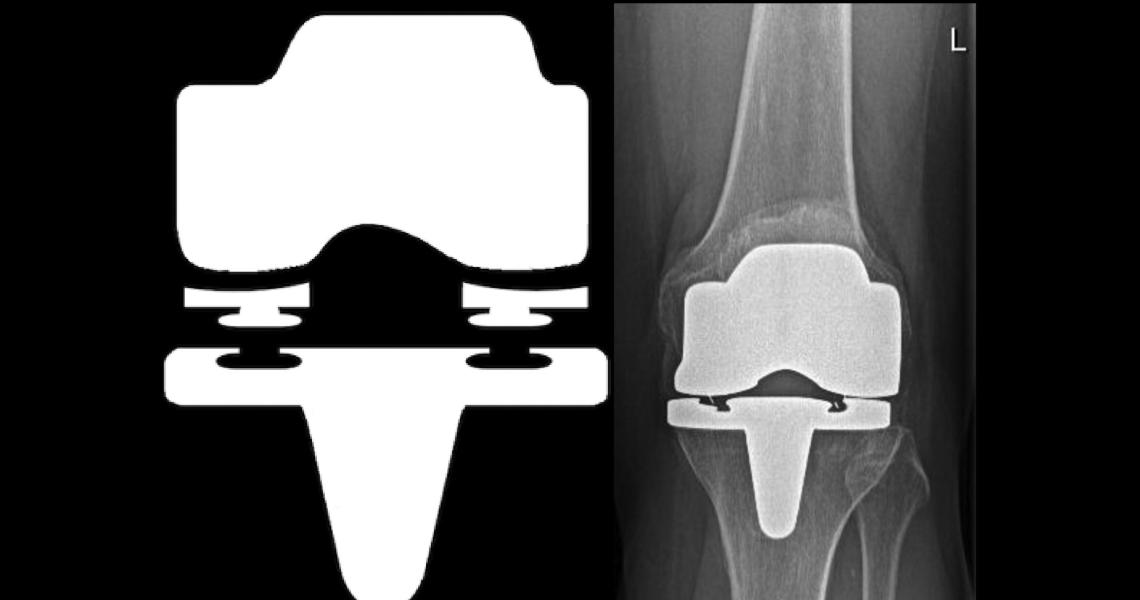
An orthopedic total joint knee replacement is not a hinge.
It bends, rolls, glides and rotates. It bears the force of walking, climbing stairs, rising from a chair and living an active life. It has to mimic naturally enough to restore function, but remain stable enough to last. Its materials must survive millions of cycles inside the body, where the smallest design decisions can affect wear, inflammation, bone loss, loosening and pain.
That was the kind of problem Michael J. Pappas ’59, ’64 helped solve.
Pappas, the late NJIT mechanical engineering professor and alumnus, collaborated with New Jersey orthopedic surgeon Frederick F. Buechel on a series of prosthetic joint innovations, including the New Jersey Low Contact Stress Knee Joint Replacement — a landmark mobile-bearing knee system that grew from a Newark-based connection between engineering and medicine.
The invention remains more than a chapter in orthopedic history. For NJIT, it is a case study in engineering’s role in health care: how a mechanical engineer and a surgeon approached the human knee as a system of motion, load, materials, geometry and biology, and how those same fundamentals continue to shape medicine today.
“The mechanical behavior of a joint replacement directly determines how well it restores function, how long it lasts, and how safely it interacts with the patient’s body,” said Robert C. Cohen ’83, ’84, ’87, chair of NJIT’s Board of Trustees and Vice President, Innovation and Technology, Orthopaedics Group, at Stryker.
Cohen’s connection to the story is personal as well as professional. Pappas and Buechel were his NJIT master’s thesis advisers for a project using finite element analysis to study fixation methods for hip joint replacement femoral stems. Cohen also worked for their company for two years while a student at NJIT.
“Every mechanical parameter — forces, materials, geometry — links directly to biological response and patient experience,” Cohen said. “Drs. Pappas and Buechel bridged mechanics and medicine so that a device not only functions mechanically, but also integrates safely and effectively with human physiology to restore a patient’s life quality.”
A collaboration built in Newark
The Pappas-Buechel partnership began in the orbit of two Newark institutions.
The work was one of the early projects in the long relationship between NJIT and the University of Medicine and Dentistry of New Jersey, now part of Rutgers. Shortly after New Jersey Medical School opened in Newark as part of UMDNJ, Pappas was asked to teach a biomechanics course. One of his students was Dr. Buechel, who later became an orthopedic surgeon and collaborated with Pappas on prosthetic joints, including the novel New Jersey Low Contact Stress Knee.
The device they developed was patented as the New Jersey Meniscal Bearing Knee Replacement. The patent lists Buechel and Pappas as inventors and describes a prosthesis that included a tibial platform, bearing inserts and a femoral component. The design addressed problems that had challenged earlier knee implants: contact stress, wear, loosening, stability, dislocation and the difficulty of preserving natural motion in an artificial joint.
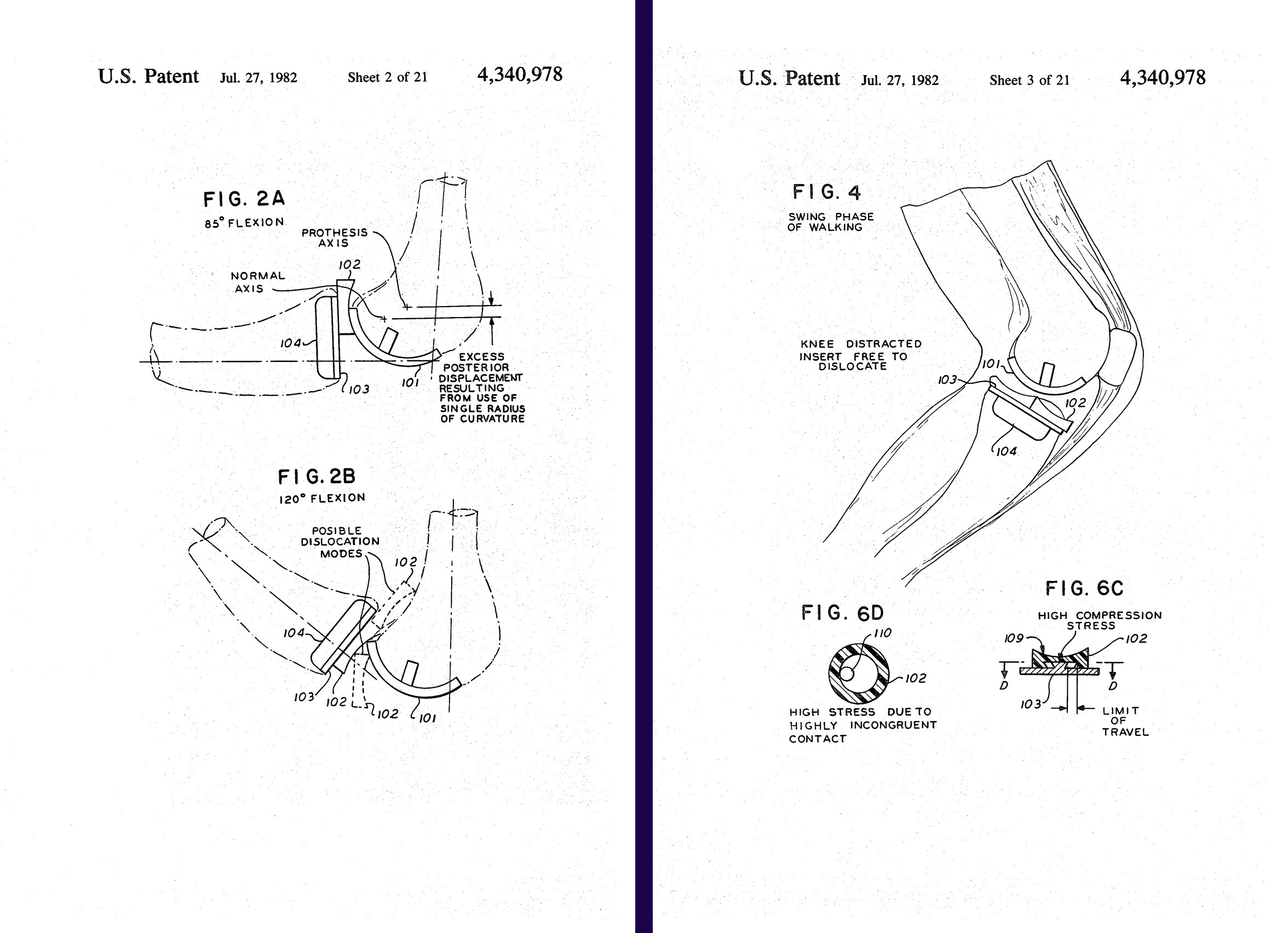
Images from the patent, filed in 1980 by the Biomedical Engineering Corp, crediting inventors Frederick F. Buechel and Michael J. Pappas.
In simpler terms, the problem was this: a replacement knee had to be stable without being overly constrained. It had to spread force across the bearing surfaces without transferring damaging loads to the bone. It had to move enough like a natural knee to support function, but predictably enough to survive inside the body.
That made it an engineering problem as much as a surgical one.
Jerry D’Alessio '93, '95, '16 senior director of applied biomechanics and advanced technology at Stryker Joint Replacement and chair of NJIT’s Newark College of Engineering Board of Visitors, said the LCS Knee remains instructive because Pappas and Buechel began with the failure modes they saw in existing designs.
At the time, many knee replacements were failing because of wear or failure of the polyethylene insert between the femur and tibia. Pappas identified excessive contact stress on the plastic bearing surface as a key driver. Increasing contact area could reduce that stress. But doing so created another problem: greater conformity could transmit torsional forces to the tibial component and contribute to loosening.
The mobile-bearing design helped address both concerns.
“By allowing the bearing to rotate, the design reduced torsional loads to frictional forces only, while maintaining maximal surface contact and lower contact stress,” D’Alessio said. “Through careful analysis of these failure modes, Drs. Buechel and Pappas developed a solution that proved durable and remained on the market for more than 40 years.”
D’Alessio’s role gives the story a present-day NJIT connection as well. As chair of the NCE Board of Visitors, he works at the same intersection the LCS Knee represents: engineering education, industry practice and invention aimed at solving real problems.
For him, the lesson is not just that Pappas and Buechel created a successful device. It is that they worked from first principles, listened across disciplines and respected what each brought to the table. Something he learned from them firsthand when, like Cohen, also worked directly with the inventors.
“The collaboration between Dr. Pappas and Dr. Buechel demonstrates the power of pairing clinical insight with engineering rigor,” D’Alessio said. “Clinicians understand the real problems that affect outcomes, while engineers bring the tools to analyze, reduce and design around fundamental failure modes.”
Orthopedic innovation looks (somewhat) different today
Digital planning, robotic-assisted surgery, additive manufacturing, artificial intelligence, advanced materials and patient-specific approaches are changing how implants are designed, planned and placed. Cohen sees those tools as powerful, but not as replacements for the engineer’s responsibility.
“What has stayed the same is the innovator’s drive and motivation to improve outcomes and the quality of care while not compromising on patient safety,” Cohen said. “Fifty years ago and today, this has not changed.”
What has changed, he added, is the capability available to engineers and surgeons.
“Digital, robotics, 3D printing and the increased power of computing combined with engineering fundamentals and material science offer us an exciting way to innovate the next generation designs and surgical tools,” Cohen said.
Still, he cautioned against mistaking the tool for the work.
“AI, robotics, and most everything else that is grabbing attention and is considered ‘game changing’ needs to be kept in its proper perspective,” Cohen said. “These things are tools. The human engineer still matters.”
That point is central to why the New Jersey Low Contact Stress Knee still resonates. Pappas and Buechel did not have today’s computing power, manufacturing methods or surgical robotics. Their work was driven by observation, mechanics, materials knowledge, clinical feedback and a willingness to rethink how an artificial knee should move inside the body.
A 2022 study in The Journal of Arthroplasty continued to evaluate the long-term performance of the uncemented meniscal-bearing cruciate-retaining LCS total knee system. In one cohort, researchers reported 92% all-cause survival and 96.7% survival for aseptic loosening after 18 years, concluding that the system demonstrated good long-term survival and functional outcomes.
I can contribute as an engineer in some way to improving tens of millions of patient lives over a career.
For a device rooted in questions of stress, wear and fixation, that long clinical history is part of the story.
For NJIT, so is the educational lineage.
The Pappas-Buechel collaboration shows what can happen when an engineer enters the medical world deeply enough to understand the patient problem, and when a clinician engages engineering deeply enough to help shape the solution. It also shows why engineering’s impact on health care is not confined to biomedical engineering alone.
Mechanical engineers understand motion, load and machine design. Materials engineers understand surfaces, wear and durability. Electrical and computer engineers shape sensors, robotics, imaging, data systems and AI. Industrial and systems engineers improve processes, safety and delivery. In modern medicine, the boundaries between those fields are increasingly porous.
D’Alessio said today’s students should see the LCS Knee as a reminder that impact begins with the problem, not the technology.
“For today’s engineering students, the key lesson is that impact comes from cross-disciplinary thinking and humility: listening to clinicians, understanding constraints, and designing solutions that work in the real world — not just on paper,” he said.
Cohen put it more directly. “The engineer owns the responsibility to create something that may remain in the human body for the rest of a patient’s life.”
“What drives me to doing this for over 40 years since my NJIT graduation?” he said. “That I can contribute as an engineer in some way to improving tens of millions of patient lives over a career. Really is such a great profession!”
The New Jersey Low Contact Stress Knee began as a response to a specific orthopedic challenge. Decades later, its broader message still holds: when engineers understand the human stakes of their work, they do more than design devices. They help medicine move.